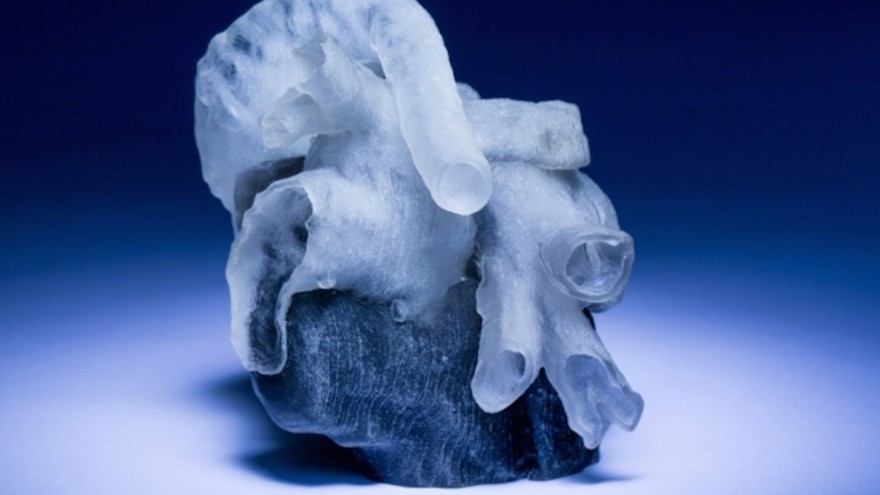
Researchers and doctors at the MIT and Boston Children’s Hospital in the United States are using MRI-scans and 3D-printing to give surgeons vivid models of human hearts. This is primarily focused on hearts shaped by defects. The underlying hope is that it would help doctors plan surgeries better and faster.
“Our collaborators are convinced that this will make a difference,” says Polina Golland, a professor of electrical engineering and computer science at MIT, who led the project. “The phrase I heard is that ‘surgeons see with their hands,’ that the perception is in the touch.”
In its current form, researchers have managed to develop an algorithm that is able to segment the image of the scanned heart, providing a fairly accurate blueprint of the patient’s heart. The 3D-printing of the model is done in a matter of hours, whereas the usual surgical planning process can take a number of days.
Seven cardiac surgeons at Boston Children’s Hospital will test the models’ usefulness around the end of this year. Each surgeon will be given data on 10 patients who have already been treated. That data will include the raw MRI scans and, on a randomized basis, either a physical model or a computerized 3-D model, based, again at random, on either human segmentations or algorithmic segmentations.
Using that data, the surgeons will draw up surgical plans, which will be compared with the surgeries already performed on each of the patients.
Cardiac surgeon Sitaram Emani is confident the physical models will improve surgical outcomes.
“We have used this type of model in a few patients, and in fact performed ‘virtual surgery’ on the heart to simulate real conditions. Doing this really helped with the real surgery in terms of reducing the amount of time spent examining the heart and performing the repair,” he told MIT.
“I think having this will also reduce the incidence of residual lesions — imperfections in repair — by allowing us to simulate and plan the size and shape of patches to be used,” Emani adds. “Ultimately, 3D-printed patches based upon the model will allow us to tailor prosthesis to patient.”