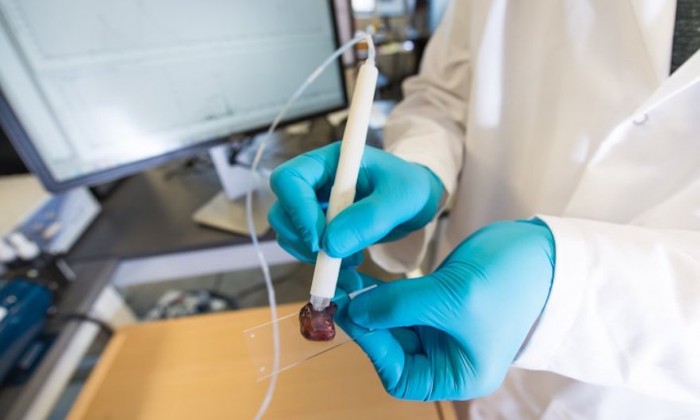
Cancer cells have a unique metabolism. Researchers at the University of Texas have managed to create a handheld device that detects their unique makeup in seconds, making sure no cancer cells are left behind during surgery.
To hear that you have cancer is scary enough. To then hear that you had an unsuccessful surgery to remove the deadly cells is even worse. Doctors are hoping to put an end to this scenario with the MasSpec Pen.
Published in Science and Translational Medicine, the MasSpec Pen helps doctors find the border between cancerous tissue and healthy tissues.
It works by releasing a tiny droplet of water on suspected cancer cells which is then sucked back into the pen for analysis. The pen is then inserted into a specially made device called a spectrometer which can measure the mass of thousands of chemicals every second.
It tells the doctors whether they are looking at cancerous cells or healthy tissues by generating a ‘fingerprint’. When the MasSpec Pen completes the analysis, the words "Normal" or "Cancer" automatically appear on a computer screen. For certain cancers, such as lung cancer, the name of a subtype might also appear.
"What's exciting about this technology is how clearly it meets a clinical need,” Livia Eberlin, an assistant professor of chemistry at the University of Texas, Austin, told the BBC. "The tool is elegant and simple and can be in the hands of surgeons in a short time."
At the moment, doctors use the Frozen Section Analysis method to test for the boundary between normal and cancerous cells. This method is slow and sometimes inaccurate. Each sample can take 30 minutes or more to prepare and interpret by a pathologist, which increases the risk to the patient of infection and negative effects of anesthesia. And for some types of cancers, frozen section interpretation can be difficult, yielding unreliable results in as many as 10 to 20 per cent of cases.
"If you talk to cancer patients after surgery, one of the first things many will say is 'I hope the surgeon got all the cancer out,' " says Eberlin. "It's just heartbreaking when that's not the case. But our technology could vastly improve the odds that surgeons really do remove every last trace of cancer during surgery."
Testing with the MasSpec Pen will continue this year as the device has already been put through its paces 253 times. In tests performed on human samples, the device was more than 96 per cent accurate for cancer diagnosis. According to Eberlin, the pen is constantly being refined to analyse smaller and smaller units of tissue but the bulky, expensive spectrometer is what’s holding the device back.
"We're envisioning a mass spectrometer that's a little smaller, cheaper and tailored for this application that can be wheeled in and out of rooms,” Eberlin was quoted as saying.
For now, the possibilities are just starting to be realised. "Any time we can offer the patient a more precise surgery, a quicker surgery or a safer surgery, that's something we want to do," says James Suliburk, head of endocrine surgery at Baylor College of Medicine and a collaborator on the project. "This technology does all three. It allows us to be much more precise in what tissue we remove and what we leave behind."




